Acute Whiplash-Associated Disorders:
Table of Contents
Acute Whiplash
Each year in America there are between 6.5 million and 7 million Motor Vehicle Accidents or (MVA’s) that affect many. Of those accidents, about three million involve some form of bodily injury. About two thirds of these injuries, while not debilitating, are permanent. When you are rear-ended your body is driven out from under your head. Although there is a great deal of soft tissue stretching that occurs in the soft tissues (LIGAMENTS, TENDONS, MUSCLES, and FASCIA), as your body travels forward at a significantly higher velocity than your head; at a certain point, these “soft tissues” cannot stretch anymore. This is the first point at which microscopic tissue tearing occurs. This is the beginning of the injury process.
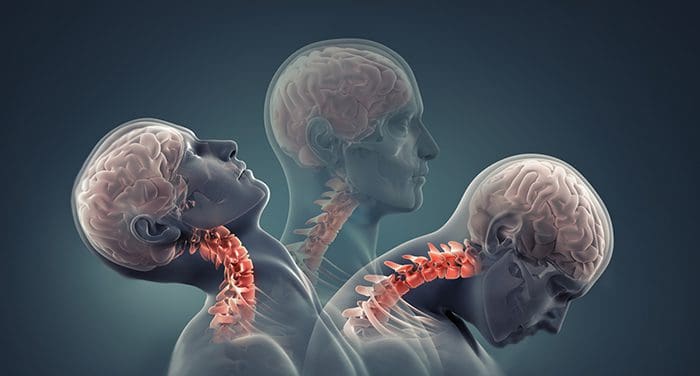
The head is now accelerating forward faster than the entire body. When the body comes to a stop (i.e. your vehicle slams into whatever is in front of it), the head will continue to travel forward. This is actually where the term “whiplash” comes from, and where it occurs. It’s exactly the principle of physics that results in the tip of a bullwhip to ‘crack’ as it breaks the sound barrier. If this type of ‘whipping’ motion occurs in the neck, it can result in a great deal of soft tissue damage and subsequent formation of fibrosis and scar tissue. Additionally, it may lead to a great deal of occult (hidden) brain and nerve system trauma.
Dr. Alexander Jimenez D.C.
Study Design:
An experimental study of motor/sensory function and psychological distress in subjects with acute whiplash injury.
Objective:
Characterizing acute whiplash injuries in terms of motor/sensory systems dysfunction and psychological distress. This involves comparison of subjects with higher and lesser levels of pain and disability.
Summary Of Background Data:
Motor system dysfunction, sensory hypersensitivity, and psychological distress are present in chronic whiplash associated disorders (WAD), but little is known of such factors in the acute stage of injury. As higher levels of pain and disability in acute WAD are accepted as signs of poor outcome, further characterization of this group from those with lesser symptoms is important.
Materials And Methods:
Motor function (cervical range of movement [ROM], joint position error [JPE]; activity of the superficial neck flexors [EMG] during a test of cranio-cervical flexion), quantitative sensory testing (pressure, thermal pain thresholds, and responses to the brachial plexus provocation test), and psychological distress (GHQ-28, TAMPA, IES) were measured in 80 whiplash subjects (WAD II or III) within 1 month of injury, as were 20 control subjects.
Results:
Three subgroups were identified in the cohort using cluster analysis based on the Neck Disability Index: those with mild, moderate, or severe pain and disability. All whiplash groups demonstrated decreased ROM and increased EMG compared with the controls (all P < 0.01). Only the moderate and severe groups demonstrated greater JPE and generalized hypersensitivity to all sensory tests (all P < 0.01). The three whiplash subgroups demonstrated evidence of psychological distress, although this was greater in the moderate and severe groups. Measures of psychological distress did not impact on between group differences in motor or sensory tests.
Conclusions:
Acute whiplash subjects with higher levels of pain and disability were distinguished by sensory hypersensitivity to a variety of stimuli, suggestive of central nervous system sensitization occurring soon after injury. These responses occurred independently of psychological distress. These findings may be important for the differential diagnosis of acute whiplash injury and could be one reason why those with higher initial pain and disability demonstrate a poorer outcome.
Sterling M1, Jull G, Vicenzino B, Kenardy J.
Author Information
Whiplash Research Unit, Department of Physiotherapy, The University of Queensland, Brisbane, Australia. m.sterling@shrs.uq.edu.au
Post Disclaimer
Professional Scope of Practice *
The information herein on "Acute Whiplash Disorders And Chiropractic Treatment Videos In El Paso, TX." is not intended to replace a one-on-one relationship with a qualified health care professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Our information scope is limited to Chiropractic, musculoskeletal, acupuncture, physical medicines, wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somatovisceral reflex clinical dynamics, subluxation complexes, sensitive health issues, and/or functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system.
Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and directly or indirectly support our clinical scope of practice.*
Our office has reasonably attempted to provide supportive citations and has identified the relevant research studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request.
We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please feel free to ask Dr. Alex Jimenez, DC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, RN*, CCST, IFMCP*, CIFM*, ATN*
email: coach@elpasofunctionalmedicine.com
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License # TX5807, New Mexico DC License # NM-DC2182
Licensed as a Registered Nurse (RN*) in Florida
Florida License RN License # RN9617241 (Control No. 3558029)
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Presently Matriculated: ICHS: MSN* FNP (Family Nurse Practitioner Program)
Dr. Alex Jimenez DC, MSACP, RN* CIFM*, IFMCP*, ATN*, CCST
My Digital Business Card



 Again We Welcome You¸
Again We Welcome You¸
