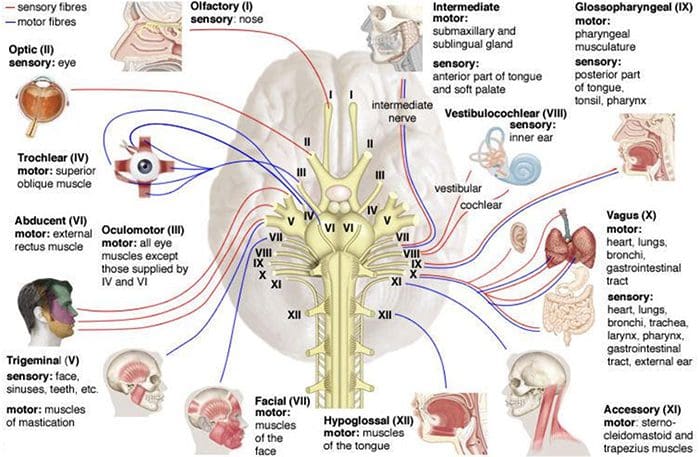
The spinal cord and brain make up the central nervous system while the spinal nerves (branching to the spinal cord) and cranial nerves (branching to the brain) make up the peripheral nervous system.
There are 31 sets of nerves that extend out of the spinal cord and are connected to it by the nerve root. Each nerve branches out about a half inch from the spinal cord before dividing into smaller branches. The dorsal rami are on the posterior side of the branch while the larger ventral rami are on the anterior side.
The dorsal rami provide nerve function for the skin of the trunk and posterior muscles. The ventral rami from T1 to T12 provide nerve function to the skin of the trunk as well as the lateral and anterior muscles.
The anterior divisions that remain for plexuses, networks that provide nerve function to the body. Each plexus has specific areas on the body for skin sensitivity as well as particular muscles. Their point where they exit the spine determines how they are numbered. The four primary plexuses are:
- Cervical plexus, C1 – C4, innervates the diaphragm, shoulder, neck
- Brachial plexus, C5 – T1, innervates the upper limbs
- Lumbar plexus, T12/L1 – L4, innervates the thigh
- Sacral plexus, L4 – S4, innervates the leg and foot.
These spinal nerves have two sets of fibers: motor and sensory. Motor fibers facilitate movement and provide nerve function to the muscles. Sensory fibers facilitate sensitivities to touch, temperature and other stimuli. They provide nerve function to the skin.

Table of Contents
What are Myotomes and Dermatomes?
A group of muscles that are innervated by the motor fibers that stem from a specific nerve root is called a myotome. An area of the skin that is innervated by the sensory fibers that stem from a specific nerve root is called a dermatome. These patterns of myotome and dermatome are almost always identical from person to person. There are occasionally variances, but that is rare.
This consistency allows doctors to treat nerve pain in patients. If a certain area is hurting, they know that it is attributed to a certain myotome or dermatome, whichever the case may be, and its corresponding nerve root. Problems with nerve damage are often the result of stretching the nerve or compressing it.
When the nerves are injured in specific areas like the lumbosacral or brachial plexus, it presents as sensory and motor deficits in the limbs that correspond to them. Myotomes and dermatomes are used to assess the extent of the damage.
How are Myotomes and Dermatomes used to Assess Nerve Damage?
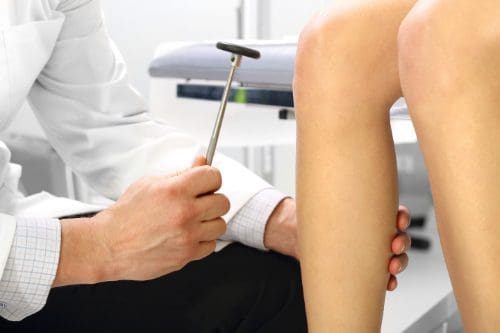
When a doctor tests for nerve root damage in a patient, he or she will often test the myotomes or dermatomes for the nerves assigned to that location. A dermatome is examined for abnormal sensation, such as hypersensitivity or lack of sensitivity.
This is done by using stimulus inducing tools such as a pen, paper clip, pinwheel, fingernails, cotton ball, or pads of the fingers. The patient is instructed to provide feedback regarding their response. Some of the abnormal sensation responses include:
- Hypoesthesia (decreased sensation).
- Hyperesthesia (excessive sensation).
- Anesthesia (loss of sensation).
- Paresthesia (numbness, tingling, burning sensation).
A myotome is tested for nerve damage in the muscles which presents as muscle weakness. This grading scale, which assigns a rating to the degree of muscle weakness, is often used:
- 5 – Normal – Complete range of motion against gravity with full resistance
- 4 – Good – Complete range of motion against gravity with some resistance
- 3 – Fair – Complete range of motion against gravity with no resistance, active ROM
- 2 – Poor – Complete range of motion with some assistance and gravity eliminated
- 1 – Trace – Evidence of slight muscular contraction, no joint motion evident
- 0 – Zero – No evidence of muscle contraction

During a typical chiropractic exam, your chiropractor will assess both dermatomes and myotomes for potential neurological problems. This gives him or her additional insight on how to treat your condition, whether it’s related to a subluxation of vertebral bodies or other other disease processes.
Back Pain Chiropractic Care | El Paso, Tx
Post Disclaimer
Professional Scope of Practice *
The information herein on "What Are Dermatomes and Myotomes? El Paso, Texas" is not intended to replace a one-on-one relationship with a qualified health care professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Our information scope is limited to Chiropractic, musculoskeletal, acupuncture, physical medicines, wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somatovisceral reflex clinical dynamics, subluxation complexes, sensitive health issues, and/or functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system.
Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and directly or indirectly support our clinical scope of practice.*
Our office has reasonably attempted to provide supportive citations and has identified the relevant research studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request.
We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please feel free to ask Dr. Alex Jimenez, DC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, RN*, CCST, IFMCP*, CIFM*, ATN*
email: coach@elpasofunctionalmedicine.com
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License # TX5807, New Mexico DC License # NM-DC2182
Licensed as a Registered Nurse (RN*) in Florida
Florida License RN License # RN9617241 (Control No. 3558029)
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Presently Matriculated: ICHS: MSN* FNP (Family Nurse Practitioner Program)
Dr. Alex Jimenez DC, MSACP, RN* CIFM*, IFMCP*, ATN*, CCST
My Digital Business Card



 Again We Welcome You¸
Again We Welcome You¸
