The first Polycystic Ovary Syndrome (PCOS) conference was held in 1990 and discussed what PCOS is and how they were diagnosing and treating patients. They looked at oligo-anovulation, no ovulation, and too many androgens. Now, we use the Rotterdam criteria. This criterion groups together anovulation abnormal ovulation, clinical hirsutism acne (signs of hyperandrogens), and an ultrasound to view the presence of 12 or more follicles and determines that if you have two out of those three then you are diagnosed with PCOS.
Table of Contents
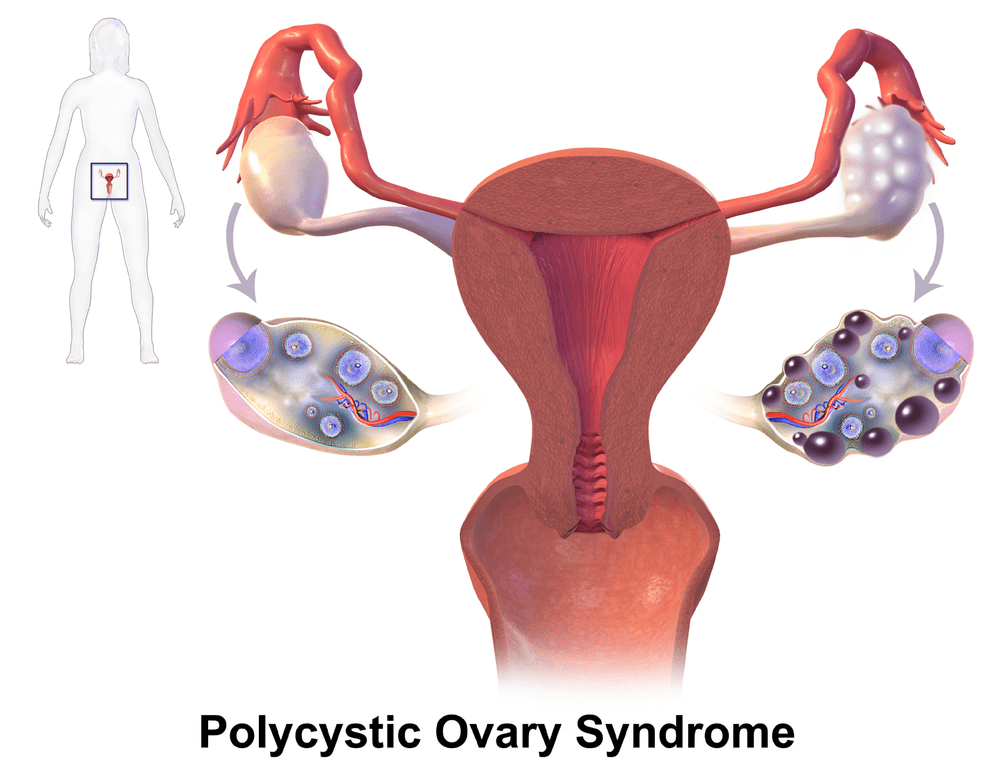
PCOS Diagnosis
When women get diagnosed they tend to have a mix of emotions. Often times they are relieved because they know what has been occurring but later they are unsure of how to proceed with their life. The biggest emotional factor when it comes to a PCOS diagnosis is fertility and the struggle it may be in the long run.
Pathway of Development
There are multiple pathways that can cause PCOS to develop. Ultimately, these pathways are categorized into 4 groups: Lifestyle induced PCOS, Poor Fat Digestion/Sugar Burner, Inflammatory Diet/Poor Food Choices, and Genetic Predisposition. Taking a look at each one we better understand what pathway our patients follow and how to approach the symptoms and diagnosis in a functional manner.
Lifestyle Induced PCOS
A major player in lifestyle-induced PCOS has to do with the Central Nervous System and an individual’s light/dark clock. As a population, we are used to a 24-7 lifestyle of constant “go”. However, if we are not getting the sunshine we need when we first wake up to stimulate our bodies into realizing its daytime and the peaceful rest we need at night to let it know it is time to heal, the circadian rhythm gets thrown off. The sun comes into the suprachiasmatic nucleus (SCN) and triggers the brain that it is daytime and time to burn energy. If you do not let your body know it is daytime then the signal does not know to store fat or burn fat, resulting in lectin production. From there, the system begins to get dysregulated. For more information on night/shift work and its impact please read the article below:
“Night Shift Work Linked To A Higher Risk Of Miscarriage”
Poor Fat Digestion/ Sugar Burner
When the lifestyle of an individual is disrupted, what we see is leaky gut. When the gut is not properly functioning we are not able to properly break down fat molecules resulting in a decrease in pancreatic elastase. Pancreatic elastase is what helps us burn fat. Next, the patient begins to create ATP (energy needed for the body to sustain its functions) out of glucose which is extremely inefficient. Patients begin to see a circle of needing to eat carbs to make glucose to make ATP for the ATP to be used up quickly and then needing to eat more carbs and so on. With this increase in carbohydrate intake and lack of energy, weight and glucose problems arise. Lastly, with dysregulation such as this, the variety of bacteria in our gut becomes reduced. This may sound like a good thing but a diverse microbiome is shown to have less inflammation and a reduced rate of disease. Without a variety of bacteria, the movement of nutrients and break down is impacted. We use the GI Effects test from Genova to properly address our patient’s inflammation, maldigestion, dysbiosis level, and bacteria variation. A sample of this test is shown below:
Inflammatory Diet / Poor Food Choices
Inflammation is a huge issue in relation to many chronic health conditions. Inflammation is a driving force in poor gut health and increased gut dysregulation. One large factor contributing to PCOS symptoms is what you eat. Our ancestors ate around 600 different foods whereas now the average human eats a very small variety, consisting of 20 foods. Gluten is often a large trigger to PCOS and inflammation as it is a non-soluble peptide. Gluten is extremely hard to digest and is hard on the gut microbiome. Prebiotics and probiotics are an excellent place to start. Kombucha is a highly effective prebiotic and when taken with a probiotic can help to increase the gut microbiome balance.
Genetic Predisposition
In specific genes, there can be SNPs (polymorphisms) and these can lead the body to have a drop in sex hormone-binding globulins which trigger luteinizing hormones in the CNS, resulting in no ovulation. Those who have SNPs are susceptible to more inflammation, environmental food triggers, autoimmune diseases, and infertility. The micronutrient test by SpectraCell provides us with insight on the methylation cycles. A sample of the test is shown below:
Additionally, for more information regarding genetic predisposition, please review the article below:
“Polycystic Ovary Syndrome: Insight into the Therapeutic Approach with Inositols”
Take-Aways
Balancing energy in the body is a fantastic place to start. This will help the body’s inflammation to become reduced overall. Secondly, reduce foods that are causing inflammatory markers. Third, assess the genetics and micronutrient variability. Last but not least, take care of the microbiome! Everything stems from the gut.
If you are having symptoms or feel as though you could have an imbalance, take the metabolic assessment below:
It is amazing when we start to truly see how many things around us cause inflammation resulting in chronic health conditions. The gut is a large factor when considering how inflammatory responses are being sent throughout the body. If you are already taking a probiotic, you can use kombucha as a prebiotic! However, be smart and safe. To start, you can mix a little kombucha with ¾ of the rest being water. This will also decrease the sugar intake. -Kenna Vaughn, Senior Health Coach
References:
Ginsberg, Dian. “5234: Functional Healing for PCOS.” Functional Medicine University. 2020, www. Functionalmedicineuniversity. com/members/1625.cfm.
Sortino MA, Salomone S, Carruba MO and Drago F (2017) Polycystic Ovary Syndrome: Insights into the Therapeutic Approach with Inositols. Front. Pharmacol. 8:341. doi: 10.3389/fphar.2017.00341
The scope of our information is limited to chiropractic, musculoskeletal, physical medicines, wellness, and sensitive health issues and/or functional medicine articles, topics, and discussions. We use functional health & wellness protocols to treat and support care for injuries or disorders of the musculoskeletal system. Our posts, topics, subjects and insights cover clinical matters, issues, and topics that relate and support directly or indirectly our clinical scope of practice.* Our office has made a reasonable attempt to provide supportive citations and has identified the relevant research study or studies supporting our posts. We also make copies of supporting research studies available to the board and or the public upon request. We understand that we cover matters that require additional explanation as how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please feel free to ask Dr. Alex Jimenez or contact us at 915-850-0900 <tel:9158500900>. The provider(s) Licensed in Texas& New Mexico
Post Disclaimer
Professional Scope of Practice *
The information herein on "Functional Wellness: PCOS" is not intended to replace a one-on-one relationship with a qualified health care professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Our information scope is limited to Chiropractic, musculoskeletal, acupuncture, physical medicines, wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somatovisceral reflex clinical dynamics, subluxation complexes, sensitive health issues, and/or functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system.
Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and directly or indirectly support our clinical scope of practice.*
Our office has reasonably attempted to provide supportive citations and has identified the relevant research studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request.
We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please feel free to ask Dr. Alex Jimenez, DC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, RN*, CCST, IFMCP*, CIFM*, ATN*
email: coach@elpasofunctionalmedicine.com
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License # TX5807, New Mexico DC License # NM-DC2182
Licensed as a Registered Nurse (RN*) in Florida
Florida License RN License # RN9617241 (Control No. 3558029)
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Presently Matriculated: ICHS: MSN* FNP (Family Nurse Practitioner Program)
Dr. Alex Jimenez DC, MSACP, RN* CIFM*, IFMCP*, ATN*, CCST
My Digital Business Card


 Again We Welcome You¸
Again We Welcome You¸
